Hereditary pancreatitis is a genetic condition characterized by recurrent episodes of inflammation of the pancreas (pancreatitis). The pancreas produces enzymes that help digest food and also produces insulin, a hormone that controls blood sugar levels in the body. Episodes of pancreatitis can lead to permanent tissue damage and loss of pancreatic function.
Signs and symptoms of this condition often begin in late childhood with an episode of acute pancreatitis. A sudden (acute) attack can cause abdominal pain, fever, nausea, or vomiting. An episode usually lasts one to three days, although some people may experience severe episodes that last longer. Hereditary pancreatitis progresses to recurrent acute pancreatitis with multiple episodes of acute pancreatitis recurring over a period of at least 1 year; the number of episodes a person experiences varies. Recurrent acute pancreatitis leads to chronic pancreatitis, which occurs when the pancreas is persistently inflamed. Chronic pancreatitis usually develops in early adulthood in affected individuals. Signs and symptoms of chronic pancreatitis include occasional or frequent abdominal pain of varying severity, flatulence, and bloating. Many people with hereditary pancreatitis also develop abnormal calcium deposits in the pancreas (pancreatic calcifications) in early adulthood.
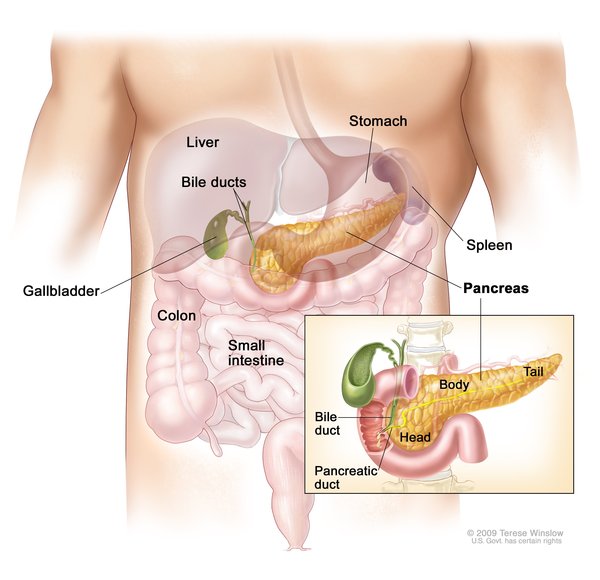
Years of inflammation damage the pancreas, causing scar tissue (fibrosis) to form instead of functional pancreatic tissue. Pancreatic fibrosis leads to loss of pancreatic function in many affected individuals. This loss of function can affect the production of digestive enzymes and disrupt normal digestion, leading to greasy stools (steatorrhea), weight loss, and protein and vitamin deficiencies. Due to a decrease in insulin production due to loss of pancreatic function, about a quarter of people with hereditary pancreatitis will develop type 1 diabetes mellitus by mid-adulthood; the risk of developing diabetes increases with age.
Chronic pancreatic inflammation and damage to the pancreas increase the risk of developing pancreatic cancer. The risk is particularly high in people with hereditary pancreatitis who also smoke, drink alcohol, have type 1 diabetes mellitus, or have a family history of cancer. In affected people who develop pancreatic cancer, it is usually diagnosed in mid-adulthood.
Complications of pancreatic cancer and type 1 diabetes mellitus are the most common causes of death in people with hereditary pancreatitis, although people with this condition are thought to have a normal life expectancy.