Limb-girdle muscular dystrophies (LGMDs) are a diverse and heterogeneous group of disorders within the broader field of genetic muscle disease. The term LGMD was first formally introduced in the 1950s to include the category of a larger group of patients with muscle weakness that could not be recognized within the major groups of muscular dystrophy identified at the time, such as muscular dystrophy of X-linked Duchenne (DMD) or facioscapulohumeral dystrophy (FSHD). In a classic article, Walton and Nattrass outlined the clinical phenotype: childhood onset of proximal weakness, slow progression, and autosomal recessive inheritance in most cases.1
Subsequently, a number of diverse conditions, including acquired inflammatory, metabolic, mitochondrial, congenital/structural, toxic, paraneoplastic, and endocrine myopathies, and even neurogenic diseases such as spinal muscular atrophy (SMA), were found to exhibit a similar clinical phenotype, which complicated and question the clinical utility of LGMD as an entity. Some authors use the term shoulder girdle syndrome to describe the clinical picture prior to the elucidation of a pathophysiological or genetic cause2,3.
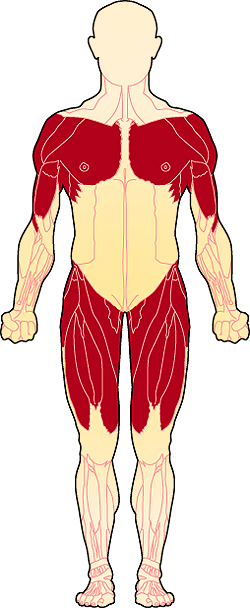
LGMD is defined as a muscular dystrophy presenting with predominantly proximal weakness, sparing facial, extraocular, and distal extremity muscles (at least early in the disease).4 According to this definition, muscle biopsy is of great importance. for inclusion in this group and also to evaluate other causes of shoulder girdle syndrome. Muscle biopsy usually shows dystrophic features, including degeneration and regeneration, increased internalized nuclei, fiber size variability, increased endomysial fibrosis, and fat replacement. However, mild and nonspecific myopathic changes can also be seen (in milder cases, earlier in the disease, or in less affected muscles) and still be consistent with a diagnosis of LGMD.5
Exact epidemiologic estimates of LGMDs are difficult to determine and vary across different populations, some due to founder effects (eg, the Amish, Libyan Jews, a Reunion Island community, among others).6–9 Using strict diagnostic criteria, some estimate a prevalence of 6 to 8 per million for autosomal recessive and sporadic cases.10 A more recent study in a population in the north of England estimated the overall prevalence of LGMD at 2.27 per 100,000.11 Autosomal recessive LGMDs they are more common than their autosomal dominant counterparts and will be discussed first in the chapter.
genetic nomenclature
The nomenclature first proposed by the European Neuromuscular Center (ENMC) workshop on LGMD4 has simply designated all autosomal dominant LGMDs as LGMD 1A, 1B, 1C, etc. and autosomal recessive LGMDs like LGMD 2A, 2B, 2C, etc. Letters indicate LGMD separated by the order of gene product identified or linked to a specific locus. The current most common LGMDs are summarized in Table 34.1.